Delay in reaching a correct diagnosis can negatively affect prognosis, since it is extremely important to treat the condition immediately. 5 Few cases have been reported in the literature as long as three weeks after surgery. Most cases appear in the early phase, developing in the first hours or days of the postoperative period 4 and manifesting as atypical cardiac tamponade. 3 Clots are limited by adhesions causing an important mass effect 1 and interfering with diastolic filling. 1 They are significantly more common after coronary artery bypass and are generally located posteriorly, 2 although compression of any cardiac chamber can occur, with right atrial involvement being the most common. Loculated hematomas with cardiac tamponade arising after cardiac surgery are a complication rarely reported in the literature. One month later he was clinically well and the echocardiogram showed no pericardial effusion, a functional biological valve and severely depressed left ventricular function. It was removed and the aortic suture was reinforced. Surgical exploration revealed a large organized pericardial hematoma compressing the right atrium. The patient was transferred to the cardiothoracic surgery center. The emergency computed tomography (CT) scan showed a hematoma measuring 9.4 cm×8.5 cm×5.9 cm compressing the right atrium and an active bleeding point 2.4 cm above the aortic prosthesis in the ascending aorta ( Figure 2A and B). The electrocardiogram showed sinus tachycardia with left ventricular hypertrophy, and the bedside echocardiogram revealed a medium-sized echogenic mass measuring 9 cm×6 cm, causing almost complete collapse of the right atrium, and mild (6 mm) circumferential pericardial effusion ( Figure 1A–D). Three weeks after surgery he suddenly became hypotensive, tachycardic, sweating, pale with cool extremities, and anuric. The patient's clinical condition improved significantly but discharge was delayed due to social problems. 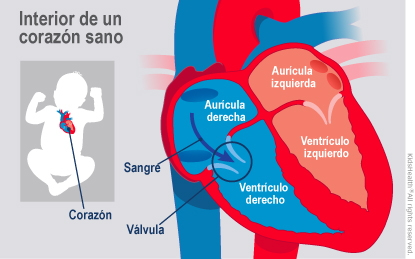 
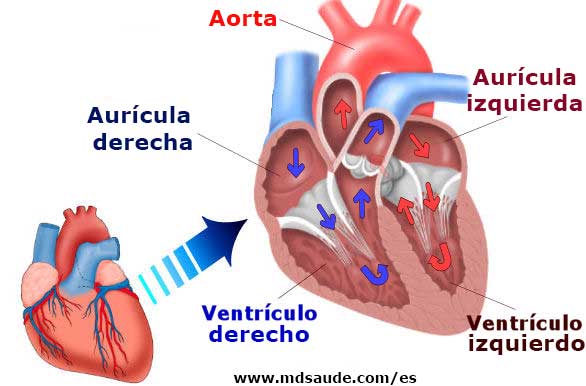
He underwent aortic valve replacement and reduction of the ascending aorta. The echocardiogram revealed a dilated left ventricle (diastolic diameter 79 mm, systolic diameter 70 mm) with severely depressed left ventricular function (20% by Simpson's method) and severe aortic regurgitation. We present a case of a 37-year-old hypertensive male admitted with dyspnea on exertion, orthopnea, paroxysmal nocturnal dyspnea, fatigue and bilateral leg edema.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
